Are patients really ‘at the centre’ of integrated care?
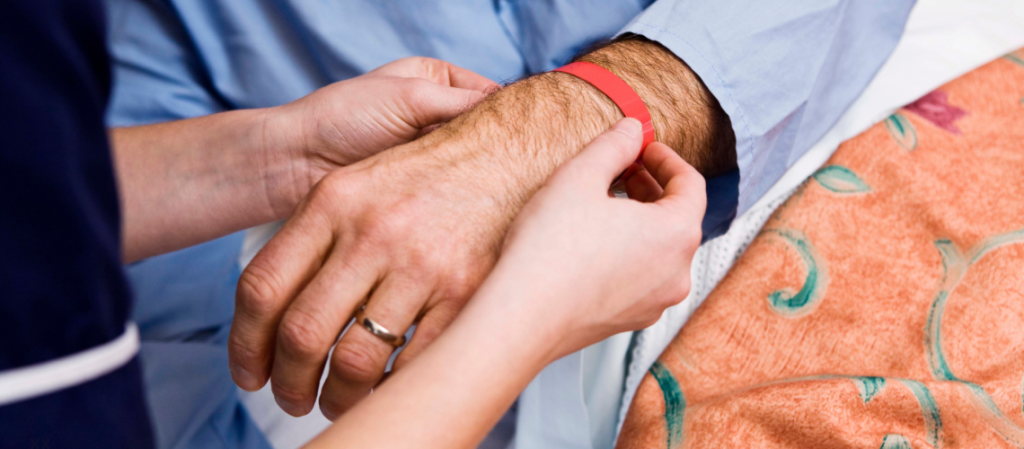
For some time now, the Government has been promoting its policy of ‘person-centred care’. In fact, the term was first introduced in the NHS Plan and other government policy documents in 2000. What is person-centred care? According to the Care Quality Commission (CQC), person-centred care is defined as ‘providers making every reasonable effort to provide […]
How to win GP contracts and funding

If you are a surgery or general practice looking to win substantial contracts or funding, it can be a daunting prospect, particularly if you are an already over-worked GP or Practice Manager struggling for time. What types of GP contracts can you bid for? APMS (Alternative Provider Medical Services) contracts are regularly put out to […]
The new CQC Framework: what is it and how will it affect providers?

Earlier this year, the Care Quality Commission (CQC) announced it would be making changes to the way it works with suppliers and providers. These changes would include the establishment of a new assessment framework and provider portal and will apply to providers, local authorities and integrated care systems. Over the course of 2023, these plans […]
K Low Consulting announces new director
We are pleased to announce that David Oakes, who has been working with us as a consultant for the last two years, has now joined the business as a company director. David brings a detailed understanding of the health and social care bidding landscape drawing directly upon roles within local government commissioning, charity, third and […]
Virtual wards: An exciting opportunity for your business
FOR many industries, the pandemic has had a lasting impact, fuelling many new opportunities for growth and change, particularly in healthcare where virtual wards are now commonly used. It’s a process which largely began during the early days of lockdown, when businesses had to react quickly to find new ways of working remotely, embracing technology […]
What is the NHS System Oversight Framework and what does it mean for procurement going forward?

At the end of June, NHS England (NHSE) announced plans to transform the way integrated care systems (ICSs) buy non NHS goods and services in a document entitled NHS System Oversight Framework 2021/22. But what is the significance of this framework? And what will it change for companies and organisations looking to land NHS contracts? […]
NHS waiting lists could result in tender opportunities
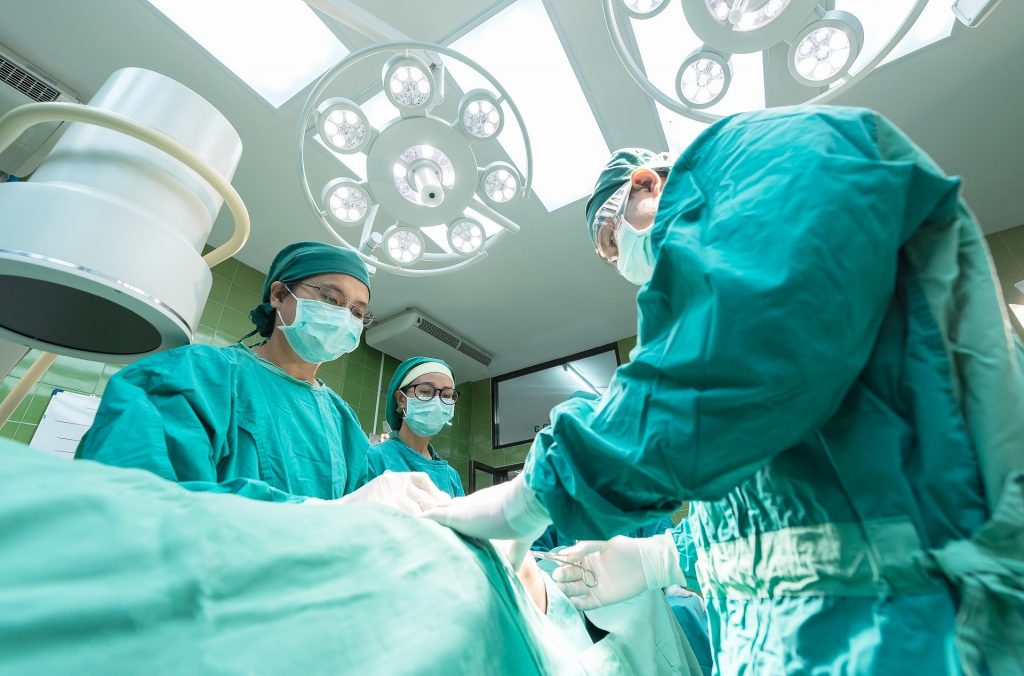
We’ve all seen the worrying headlines about the growth in NHS waiting lists following the onset of the Coronavirus pandemic. Just this week it has been reported in the national news that the number of people on NHS waiting lists hit a 12-year high. At least 162,000 patients are waiting more than a year for […]
NHS England- PDPS Contract Announcement

NHS England’s PDPS APMS Contract Announcement NHS England’s PDPS APMS Contract has now been released on January 23rd and encourages all GP providers who wish to bid in the future, to apply as soon as possible. In case you haven’t seen our previous blog posts about the contract, the APMS PDPS Contract was announced in […]
Looking ahead to 2020: A successful year for K Low Consulting

Reflection on 2019 We’ve had a great year at K Low Consulting and are excited about the new year ahead! In this article, our team reflects on 2019 and looks ahead to the future of K Low Consulting. In 2019, we have experienced significant and rapid growth. We have expanded our associate team, which includes […]
To Bid or Not to Bid: A Step Towards Winning a Tender

The tender process is often complex and requires close attention to the contract requirements and your organisations’ suitability to a contract. As part of our services at K Low Consulting, we help clients to make a ‘bid or no bid’ decision in the initial stages of bidding. This often includes evaluating compliance and eligibility, commercial […]
