What does the abolition of NHS England mean for NHS procurement?

On March 13, 2025, the Government announced the abolition of NHS England. The Government says this move is being made to streamline healthcare management by integrating NHS England’s functions directly into the Department of Health and Social Care (DHSC) and it ‘will reduce bureaucracy, make savings and empower NHS staff to deliver better care for […]
NHS tenders: What rule changes are coming into force in 2025?

This year, the NHS is making wholesale changes to the way businesses can procure tenders. The Procurement Act 2023, is set to come into force at the end of February and with it comes changes that aim to make the process more streamlined; enhancing transparency and making for a more level (and competitive) playing field. […]
Are patients really ‘at the centre’ of integrated care?
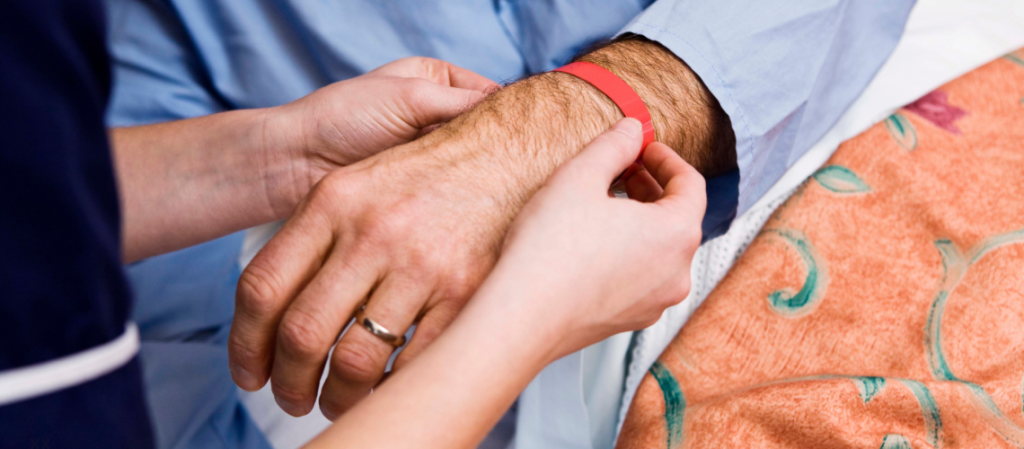
For some time now, the Government has been promoting its policy of ‘person-centred care’. In fact, the term was first introduced in the NHS Plan and other government policy documents in 2000. What is person-centred care? According to the Care Quality Commission (CQC), person-centred care is defined as ‘providers making every reasonable effort to provide […]
Are you able to demonstrate your Carbon Reduction Plans in a tender bid?

From April 2024, it will be compulsory to demonstrate Carbon Reduction Plans (CRPs) in any NHS tender bid submissions. This is because the NHS has announced a goal to achieve net zero emissions by 2045 and this will also include emissions generated by goods and services purchased through its suppliers. Since April 2023, for all […]
The new CQC Framework: what is it and how will it affect providers?

Earlier this year, the Care Quality Commission (CQC) announced it would be making changes to the way it works with suppliers and providers. These changes would include the establishment of a new assessment framework and provider portal and will apply to providers, local authorities and integrated care systems. Over the course of 2023, these plans […]
New bill will make it easier for businesses to compete for public sector contracts
A new bill is currently being passed through Parliament which aims to make it easier for businesses to enter public sector supply chains. The Procurement Bill lays out new rules and procedures for central government departments, their bodies and the wider public sector when selecting suppliers and awarding contracts with a value above certain thresholds. […]
Virtual wards: An exciting opportunity for your business
FOR many industries, the pandemic has had a lasting impact, fuelling many new opportunities for growth and change, particularly in healthcare where virtual wards are now commonly used. It’s a process which largely began during the early days of lockdown, when businesses had to react quickly to find new ways of working remotely, embracing technology […]
Integrated care systems – what direction are things moving in?
In 2019, the NHS set out plans to revolutionise Integrated Care Systems (ICSs) as part of its Long Term Plan. The proposals included: Giving people more control over their own health and the care they receive Encouraging more collaboration between GPs, their teams and community services, as ‘primary care networks’ to increase the services they […]
What is the NHS System Oversight Framework and what does it mean for procurement going forward?

At the end of June, NHS England (NHSE) announced plans to transform the way integrated care systems (ICSs) buy non NHS goods and services in a document entitled NHS System Oversight Framework 2021/22. But what is the significance of this framework? And what will it change for companies and organisations looking to land NHS contracts? […]
Waiting lists and the long-term future of the NHS

Healthcare waiting lists in the UK are reported to be longer now than they have been for about two decades. In total, 4.52 million people are currently on NHS waiting lists and around 224,000 patients have been waiting for longer than a year. Experts have warned the overall waiting list figure could double to as […]
